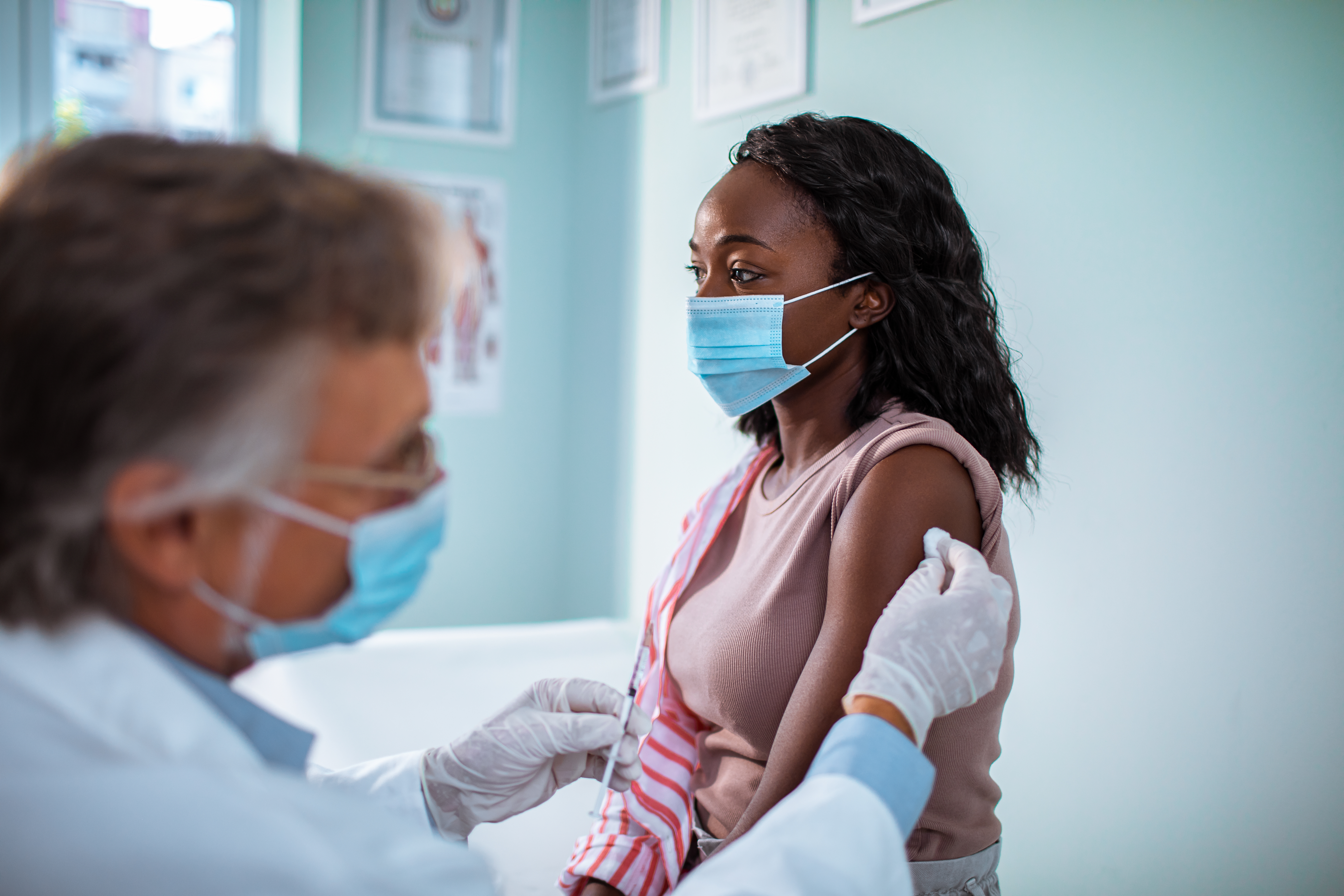
COVID-19 Vaccine, Testing, and Treatment Commercialization
COVID-19 Vaccine, Testing, and Treatment Commercialization
This updated Flash on the newly FDA-approved COVID vaccine reflects new market changes in addition to corrections regarding rates and cost noted below.
Updates
- On September 11, 2023, the US Food and Drug Administration (FDA) approved updated coronavirus disease 2019 (COVID-19) vaccines targeting more currently circulating variants. The FDA has indicated that the composition of COVID‑19 vaccines may require annual updates similar to the seasonal flu vaccine. The updated mRNA vaccines have FDA traditional approval for patients 12 years of age and older and have emergency use authorization (EUA) for individuals six months through 11 years of age. As a result of the approval of the updated vaccines the previously approved bivalent Moderna and Pfizer-BioNTech COVID‑19 vaccines are no longer authorized for use in the United States.
- Following the FDA approval the Centers for Disease Control and Prevention (CDC) recommended the updated vaccines for everyone six months and older.
- Communications from the US Department of Health and Human Services (HHS) have indicated that following cessation of the government supply of COVID-19 vaccines, the cost of the vaccine is expected to be borne by the Vaccines for Children (VFC) Program for most children enrolled in Medicaid. Communications from the CDC did not specify that an EUA approved vaccine would have different VFC coverage than a traditionally approved vaccine.
Corrections
- Centers for Medicare & Medicaid Services (CMS) indicated they will align the COVID-19 vaccine Medicare administration rate with the rate for other Part B preventative vaccines effective January 1 of the year following the year in which the EUA for COVID-19 ends. The end of the EUA has not yet been determined. The EUA declaration is distinct from the COVID-19 public health emergency (PHE). Mercer had previously indicated the Medicare vaccine administration rate for COVID-19 vaccines would be lowered to align with payment rates for administering other Part B preventive vaccines effective January 2024.
- Following the commercialization of the COVID-19 vaccine, the cost of the COVID‑19 vaccine for Medicaid enrolled children is expected to be covered by the VFC program. For Children’s Health Insurance Programs (CHIP) enrolled Medicaid children, states would be required to cover the cost of the COVID-19 vaccine after the government no longer supplies doses.
Overview
“Commercialization” refers to the transition from federal purchase of COVID-19 vaccines, testing and treatments to payers, including state Medicaid, CHIP, VFC, and private payers. Commercialization of COVID-19 vaccine, testing, and treatment will occur in the fall of 2023 following the recent end to the PHE and a depletion of the federally‑purchased supply.
Considerations for State Medicaid and CHIP Programs
State Medicaid programs should evaluate how to best manage the commercial transition to Medicaid and CHIP in the fee-for-service and managed care environments.
In particular, states should consider:
COVID-19 Vaccines
- HHS indicated vaccine ordering through the US government will begin to phase out beginning August 3, 2023; transition to the commercial market will occur in mid-to-late September 2023 following the FDA and CDC approval of the updated vaccines.
- Vaccine Ingredient Cost: Medicaid programs and CHIP are required to cover COVID‑19 vaccines and boosters with no cost sharing. This includes the ingredient cost following the end of the supply of federally‑purchased vaccines.
- The manufacturers of the vaccines have indicated an anticipated price of approximately $130 per dose.
- For pediatric (under age 19) Medicaid enrollees, vaccine ingredient cost would be federally supplied under the VFC program, leaving state Medicaid programs only responsible for the cost of administration for pediatric patients. For CHIP enrolled Medicaid children, states would be required to cover the cost of the COVID-19 vaccine after the federal government no longer supplies doses.
- For adult patients (ages 19 and up), state Medicaid programs will be responsible for both the ingredient cost and administration cost.
- Medicaid programs and CHIP are required to cover COVID-19 vaccines approved under an Emergency Use Authorization (EUA) or approved by the FDA without cost sharing through September 30, 2024. Afterwards, they will only be required to cover FDA-approved vaccines without cost sharing.
- Federal Claiming: States will receive 100% federal matching payments for the COVID-19 vaccine ingredient through September 30, 2024. Afterwards, these costs will be matched at the state’s regular and enhanced (for CHIP) federal match rate. States that include these costs in capitated Medicaid managed care may need an updated methodology for claiming enhanced federal match.
- COVID-19 Vaccine Administration Cost
- During the PHE, many states tied the COVID-19 vaccine administration payment rate to the Medicare payment rate ($40). CMS has not yet specified the date when they plan to lower the COVID-19 vaccine Medicare administration rate.
- States that have tied the COVID-19 vaccine administrative rate to the Medicare rate in their State Plan through September 30, 2024 could return to using the state’s regular vaccine administration fee or establish a new policy in the State Plan, beginning October 1, 2024.
- Federal Claiming: States will receive 100% federal matching payments for the costs associated with administering the vaccine through September 30, 2024. At that time, state costs will be matched at the state’s regular Federal Medical Assistance Percentages (FMAP) and enhanced (for CHIP). States that include these costs in capitated Medicaid managed care may need an updated methodology for claiming enhanced federal match.
COVID-19 Testing
- State Medicaid programs and CHIP must cover COVID-19 over-the-counter (OTC) and laboratory testing services for enrollees at no cost through September 30, 2024.
- OTC Costs
- Medicare has discontinued coverage of OTC tests, although some Medicare Advantage plans may be continuing coverage that will be available to dual eligibles.
- State Medicaid and CHIP programs will need to maintain OTC coverage through September 30, 2024, but do have flexibility their coverage policy to reflect the end of the PHE.
- Continued market entry of OTC testing products is expected to lower unit costs for OTC testing.
COVID-19 Treatment
- Medicaid programs and CHIP are required to cover all drugs and biological products for the treatment or prevention of COVID-19 with no cost sharing for enrollees September 30, 2024.
- After September 30, 2024, FDA-approved treatments are required to be covered; however, states may implement cost sharing requirements and appropriate utilization limits. Non‑FDA approved treatments approved only under EUA coverage may vary based on individual state decisions.
- The federal government purchased 24 million courses of Paxlovid™, Pfizer’s oral antiviral COVID-19 treatment, with supply expected to run out in 2024. Following depletion of government-purchased treatments, state Medicaid programs will be responsible costs of the medications as well as any associated administration or dispensing costs. These state Medicaid and CHIP costs will be matched at the state’s regular and enhanced (for CHIP) FMAPs.
References
CDC Recommends Updated COVID-19 Vaccine for Fall/Winter Virus Season | CDC
COVID-19 Commercialization | HHS.gov
Commercialization of COVID-19 Vaccines, Treatments, and Tests: Implications for Access and Coverage ꟾ Kaiser Family Foundation
Medicare COVID-19 Vaccine Shot Payment | CMS
Want to download this FLASH?
Is this content exactly what you need and you are interested in downloading the document? Feel free to click below to save a PDF of the contents.
Questions for your specific state?
Please contact Meredith Mayeri, Dr. Bethany Holderread, or your Mercer consultant to discuss the impact of these changes to your specific state programs. You may also email us at mercer.government@mercer.com.
View more information at https://www.mercer.com/government

Caveats and limitations
Mercer is not engaged in the practice of law, or in providing advice on taxation matters. This report, which may include commentary on legal or taxation issues or regulations, does not constitute and is not a substitute for legal or taxation advice. Mercer recommends that readers secure the advice of competent legal and taxation counsel with respect to any legal or taxation matters related to this document or otherwise.
New Drug Update - August 2023
Discusses gene and cellular therapies, biosimilars, oncology, FDA new drug approval patterns, and more.
Stay informed
Subscribe to updates on public health, Medicaid and other critical topics for states.